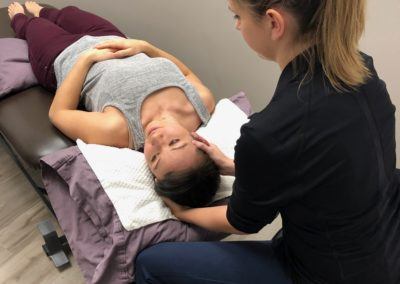
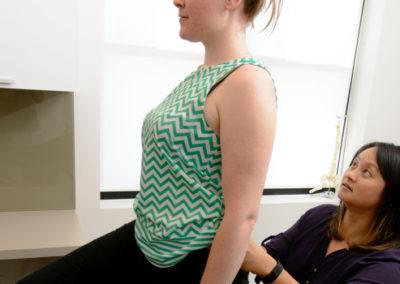
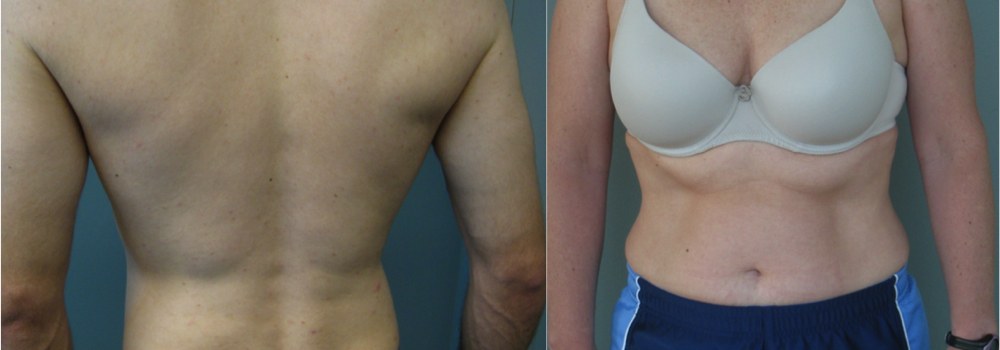
Back pain happens to everyone and for some is a life-changing occurrence.
 The causes are as many as there are structures capable of producing pain; and every tissue in the body is capable of giving us pain. Help from the health care profession is sought when the pain is severe enough to interfere with activities we need, or want to do. What happens next depends on who you choose to consult.
The causes are as many as there are structures capable of producing pain; and every tissue in the body is capable of giving us pain. Help from the health care profession is sought when the pain is severe enough to interfere with activities we need, or want to do. What happens next depends on who you choose to consult.
There are many health care practitioners who treat back pain – the family doctor, chiropractor, physiotherapist, massage therapist, acupuncturist, orthopaedic surgeon, neurosurgeon, anesthetist, rheumatologist, psychiatrist and psychologist to name but a few. Each approaches your problem from a very different perspective, which is based on their formal training and their clinical experience. Their training/experience helps them to develop models some of which are based on scientific principles and some on long time common thought.
Back pain has been the subject of significant scientific research, so what does the research tell us. First of all consider the questions we have asked in the research. It’s important to understand the question because it ultimately directs the answer. If one is interested in understanding “What structure is responsible for an individual’s pain?” then the research will focus on specific anatomical parts capable of generating pain. Entire models for both assessment and treatment of the low back have been developed following this line of questioning. Highly sophisticated imaging techniques and surgical procedures have been developed to address this question – “What is hurting”? This would be useful clinically if only one structure was responsible for an individual’s pain. Unfortunately, multiple structures are often the problem and it is not possible to identify them individually. So we see diagnoses such as ‘non-specific low back pain”. In other words, the pain is not specific to any identifiable structure; however, your low back pain is acknowledged. Even if we did know what structure was responsible for the pain, this would not help us in treatment unless all we wanted to do was cut it out or numb it with an anaesthetic – sometimes this is necessary but rarely is this all that is needed.
What information would be gained if the initial research question was “Why is the low back or pelvis painful?” “Why is the back no longer able to sustain or transfer the loads, stand, sit, lift or twist?” To answer these questions, the research must explore how the region functions in order to appreciate why breakdown and pain have occurred. Much research has been done with these questions in mind and today we use The Integrated Systems Model, which considers not only the behaviour of your pain but you how your whole body is functioning and how the multiple impairments are in relationship and whether that relationship is responsible for your back, or pelvic, pain.
Living on Earth means that we are never able to escape the influence of gravity. Being upright (bipedal) requires that the gravitational forces be transferred through the low back and pelvis to the two legs. How effective we are at managing this load over a lifetime dictates how well we can stand at ease, move at will and react when necessary as we age, in other words how well we function. Dysfunction implies that the individual has lost the ability to resist gravity while standing, sitting, lifting etc. Transferring loads effectively, whether the load is merely our body weight or the addition of extra loads (groceries, children, tool boxes etc), requires proper function of the bones, joints, muscles and nerves. Collectively, all of these systems must be working together to produce smooth effortless movement. The bones can’t be broken or effected by disease, the joints must be mobile and yet their motion controlled, the muscles must be strong and flexible to support us while not limiting movement and the nerves must act as a highly sophisticated information system coordinating multiple functions at the same time.
Beautiful movement is like beautiful music; each muscle is like an instrument in the orchestra and must be trained individually. However, beautiful music can only be heard when the conductor orchestrates the individual instruments – you play more, you play less, you be quiet. The nervous system is the conductor for our muscles and training the conductor is what we refer to as motor control training. You cannot strengthen a muscle that the brain is not using, therefore motor control core training must come before core strengthening. This is true for all areas of the body, not just the low back and pelvis.
Gravity tries to push us into the ground and this force is called compression. Compression forces the bones of your back together and this force is naturally resisted by the structure of the joints and also the intervertebral discs. When your back is under more compression than it can handle, in other words when it is not being supported by the muscle system, the discs and joints begin to show signs of wear and tear – a naturally occurring event that doesn’t have to be associated with pain or aging, but sometimes is.
The doctor may look at your X-ray, see structural changes in your spine, note your age then tell you that you have “degenerative disc disease”. This is more often not a disease but rather a statement indicating that you have fallen victim to the compressive force of gravity and haven’t been using your muscle system well enough to counteract it. The structures of your back are showing the signs of too much compression and telling you about it by sending your brain signals that it interprets as pain. There are just as many people on this planet who have the same changes in their spine on imaging as you do and do NOT have pain. Pain and structural changes on imaging do NOT always corelate – they have to match the clinical picture so don’t get too caught up in your imaging results unless they match your story!
How does the muscle system resist gravity and the extra loads we apply to our bodies yet still allow us to move? According to motor control theory, the nervous system orchestrates exactly the right amount of muscle contraction, at the right time for the task you are doing. The net result of this co-activation of muscles is that you are supported, yet still able to move, you have ‘stability’, or control, as well as mobility.
Let’s talk a bit about this muscle system that is orchestrated by the nervous system. It has long been thought that a strong abdomen helps to relieve back pain. While true in part, it’s not quite so simple, situps are not the cure for back pain. The word ‘core’ is used in both the research and training literature to mean many different things, what is the core?
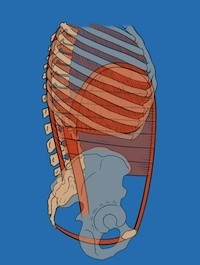
Your core is located between the breathing diaphragm, pelvic floor, abdominal wall (both deep and superficial parts) and back muscles. Research has found that retraining the timing of contraction (synergy) of these muscles is important for restoring function to this region of the body. Creating neural networks for using this system automatically and efficiently (as opposed to strongly) is the initial goal. This is called core training and again, you cannot strengthen a muscle that your brain is not activating. Once your mind can connect properly to the deeper aspects of this canister, core strengthening exercises are appropriate. If you begin a core strengthening program without first addressing the sequencing and timing of the muscles you’re attempting to strengthen, you will likely reinforce the non-optimal patterns you have. If you always do what you’ve always done, you’ll always get what you’ve always got.
Read the education article Motor control core training vs core strengthening to learn more about the deep muscles of the core and how we train before adding strengthening exercises.
When all of these muscles are performing properly you have a core of support that allows your hips to swing freely as you walk and run. In addition, when the core is working well, your chest will not be gripped or braced and you will be able to breathe easily and be free to rotate or twist your chest.
So where do you go from here. Ask yourself this question – Have I been seeking a structural diagnosis i.e. What is hurting? Do I truly understand my own muscle system and how I use this to support my back, pelvis and chest (thorax)? Do I pay attention to this deep muscle system when sitting, standing, lifting twisting or just use any strategy that comes to me? If you have back pain, you can’t do this anymore.
It is never too late to improve your function. Give us a call, we’d love to help get you back on track to living with an active, healthy body.